Using Your Benefit Convenience Card
Summary

Healthcare Cost Assistance benefits cover 100% of net monthly premiums for your individual Marketplace plan, or a portion of your Medicare premiums. These benefits also provide funds for out-of-pocket medical expenses for claims covered by your approved Marketplace plan, Medicare, VA benefits, CHAMPVA, or TRICARE.
You manage these benefits with your Benefit Convenience Card (BCC). The BCC is a Mastercard credit card, mailed to you and administered by Ameriflex.
Your BCC works just like a regular credit card, except that:
- Your card is limited in use to Marketplace premium payments and covered out-of-pocket medical expenses for a Carewell-approved Marketplace plan, Medicare, VA benefits, CHAMPVA, or TRICARE. Covered medical expenses include deductibles, copayments, and coinsurance expenses, such as covered prescriptions.
- Since the BCC is only for covered medical expenses, you may need to show proof of your covered out-of-pocket expenses. Please keep your Explanation of Benefits (EOBs) and receipts. It’s important to keep your itemized prescription receipts since prescription expenses may not appear on your insurance carrier’s EOBs.
The BCC can’t be used for: You may be financially responsible for repaying funds to Carewell SEIU 503 if your card is used for expenses that are not covered medical expenses.
Important Note: The source of truth for all Carewell rules and guidelines—including instructions for using your BCC—is covered in the Guide to Carewell Training and Benefits. When a discrepancy is identified between Carewell guidelines and those of Carewell’s vendor partners (Ameriflex), Carewell guidelines will override vendor rules.
One of the best things about the BCC is that if you are enrolled in an individual Marketplace plan, you can set up autopay and make sure your premium is paid on time every month.
Contact your Marketplace insurance carrier to set up automatic payments from your Benefit Convenience Card:
- Kaiser: Visit the Kaiser Permanente website.
- PacificSource: Visit the PacificSource website.
- Providence: Call Providence billing at 1-503-574-5791 or pay your premium online — for first time premium payments, use this link and select New individual & family applicants.
- Regence: Customer Service 1-888-675-6570 / Regence website / To create an account, go to www.regence.com/member/registration.
What can you use the Benefit Convenience Card for?
For phones, scroll left to view the rest of the table.
| Monthly premiums | Out-of-pocket expenses* | |
| Approved Marketplace Plan Click here for more information. | YES! [Exceptions may apply, see below] Contact your insurance carrier to set up automatic premium payments with your card. | YES! Covered medical expenses (up to the annual BCC allowance): – The deductible on your approved Marketplace plan – Medical copayments and coinsurance expenses, including for covered prescriptions |
| Medicare Click here for more information. | NO. You will need to use the reimbursement process for your Medicare premium(s). | YES! Covered medical expenses (up to the annual BCC allowance): – Deductibles on your Medicare coverage – Medicare copayments and coinsurance expenses, including for covered prescriptions |
| VA Benefits, CHAMPVA, TRICARE Click here for more information. | NO. VA benefits, CHAMPVA, and TRICARE premiums are not covered under HCA. | YES! Covered medical expenses (up to the annual BCC allowance): – Deductibles on your Military Connected health plan – Military Connected health plan copayments and coinsurance expenses, including for covered prescriptions |
*The BCC out-of-pocket account can only be used for the items listed above. Because your BCC only covers eligible medical expenses, this list may differ from the card uses listed on the Ameriflex website or in the notice you get from Ameriflex when you receive your card. For example, the BCC can’t be used at the FSA Store or for any medical expenses not covered by your insurance plan. If you use the BCC for any unauthorized expenses, you may need to repay Carewell SEIU 503 for these charges.
Marketplace Exceptions
- If your family is included on your health insurance plan, or
- If you receive the temporary Healthcare Cost Assistance benefit
In both cases, you may still use the BCC for your personal covered out-of-pocket expenses. However, you must pay your premium directly to your insurance carrier using your own funds and then submit a Medical Premium Reimbursement Claim Form to Carewell SEIU 503. Once your reimbursement request has been processed, you will receive a check for the amount of your premium.
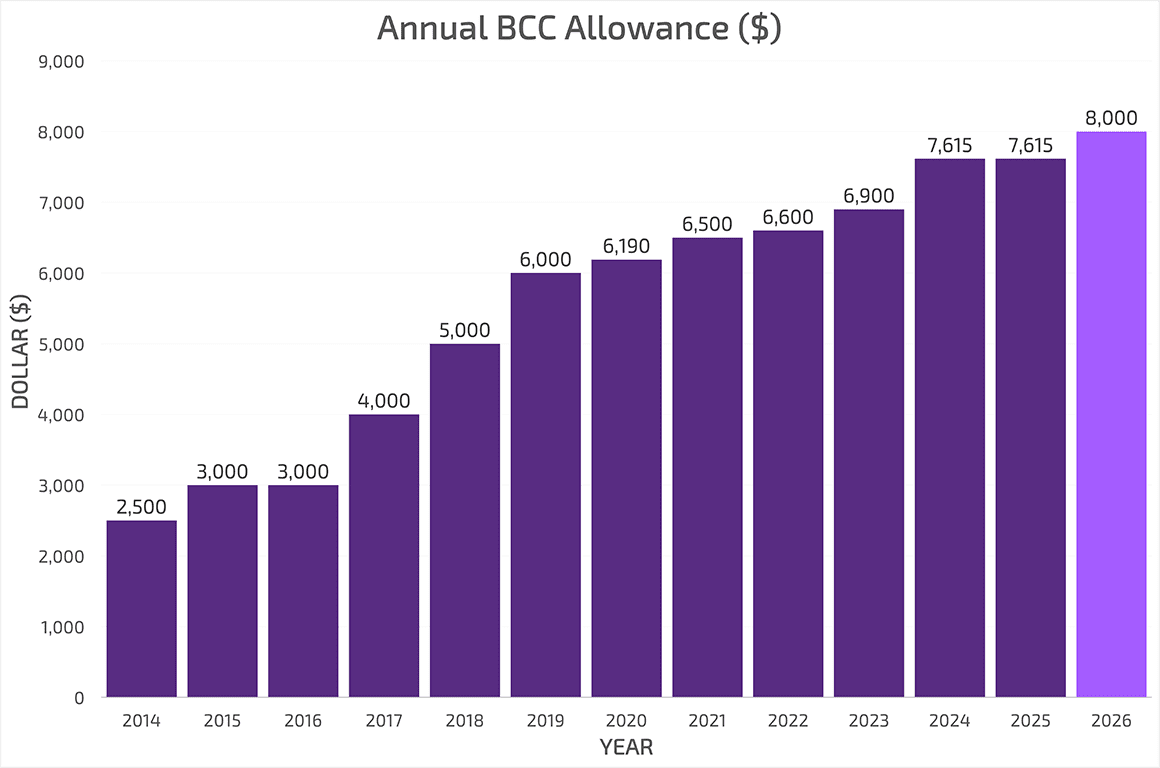
How much money is on the BCC?
There are 2 separate accounts on your BCC: 1 for paying your premiums (if applicable), and 1 for covered out-of-pocket medical expenses.
This chart shows the amount available for the annual BCC allowance for covered out-of-pocket medical expenses since the start of this program.
Submit a claim for reimbursement from Ameriflex (BCC Administrator)
Submit a claim for reimbursement from Ameriflex for:
- Covered medical out-of-pocket expenses if you paid with your own funds.
- Covered Medicare out-of-pocket expenses if you paid with your own funds.
- Covered VA Benefits, CHAMPVA, or TRICARE out-of-pocket expenses if you paid with your own funds (reimbursements back to January 1, 2026, IF you were eligible for Healthcare Cost Assistance at the time).
- Net monthly medical premium for approved individual plans purchased through the Marketplace paid for with your own funds (not family plan, not temporary Healthcare Cost Assistance reimbursement).
- Services received in the previous year, submit a reimbursement form to Ameriflex for services received up to 12 months back, if you were eligible for Healthcare Cost Assistance at the time. (Does not include VA Benefits, CHAMPVA, or TRICARE for 2026.)
For all BCC expenses, you must submit proof to Ameriflex. Please keep your Explanation of Benefits (EOBs). It’s also important to keep your itemized prescription receipts since prescription expenses may not appear on your insurance carrier’s EOBs. If you don’t submit proof of all BCC expenses to Ameriflex, you may need to repay Carewell SEIU 503 for these charges.
Connect with Ameriflex!
Managing your Benefit Convenience Card is easy!
There is a Quick Link to your Ameriflex account on your MyCarewell503 dashboard.
If you haven’t already logged in to your account on MyCarewell503, follow this link:
-
- Once you sign in, on the right column of your dashboard, click on Ameriflex under QUICK LINKS
- You are taken directly to your personal account on Ameriflex from your MyCarewell503 dashboard
- All the Ameriflex setup information is instantly available to connect to Ameriflex
You can use the Ameriflex online portal to:
-
- check the balance on your Benefit Convenience Card (BCC)
- connect your health plan account
- MyPlanConnect automatically locates the Explanation of Benefits (EOB) for your transaction to provide the required documentation of charges for Ameriflex
- view your payment history
- submit claims online
- update your reimbursement method
- see the status of a reimbursement
- order a replacement card
3 steps to make managing your BCC payments easier
Create an Account
Create your account at myameriflex.com.
Set up and use MyPlanConnect.
If you use your BCC, MyPlanConnect automatically locates the Explanation of Benefits (EOB) for your transaction, and you won’t need to submit further documentation.
See details and directions at https://myameriflex.crunch.help/participants/Setting-Up-and-Using-MyPlanConnect.
Download App
Once you’ve set up your account, download the MyAmeriflex mobile app at myameriflex.com/participants/the-ameriflex-difference/mobile-app. The Ameriflex app lets you access and manage your account on the go!
Ameriflex resources
Accessing the Ameriflex portal and MyPlanConnect
Accessing the Ameriflex Mobile App
Other Ameriflex resources
Contact Ameriflex
Ameriflex representatives are also available to assist on the phone Monday through Friday 5am to 6pm, and Saturday 7am to 11am (PST) at 1-888-868-3539.